Medicare Will Cover Lymphedema Compression Treatment Items
- oralie

- Jan 4, 2023
- 3 min read
Updated: Feb 28, 2023
One in 1,000 Americans suffer from lymphedema - swelling in an arm or leg caused by a lymphatic system blockage. Surgery for cancer, older age, excess weight, and venous diseases are all risk factors. Many readers probably know someone that is suffering from lymphedema in silence or you may suffer from lymphedema yourself and understand the struggle to access lymphedema compression treatments under Medicare. Traditionally, accessing lymphedema compression treatment supplies has been a real challenge for individuals, and for many physical therapists, occupational therapists, and physicians but we are here to share some good news!
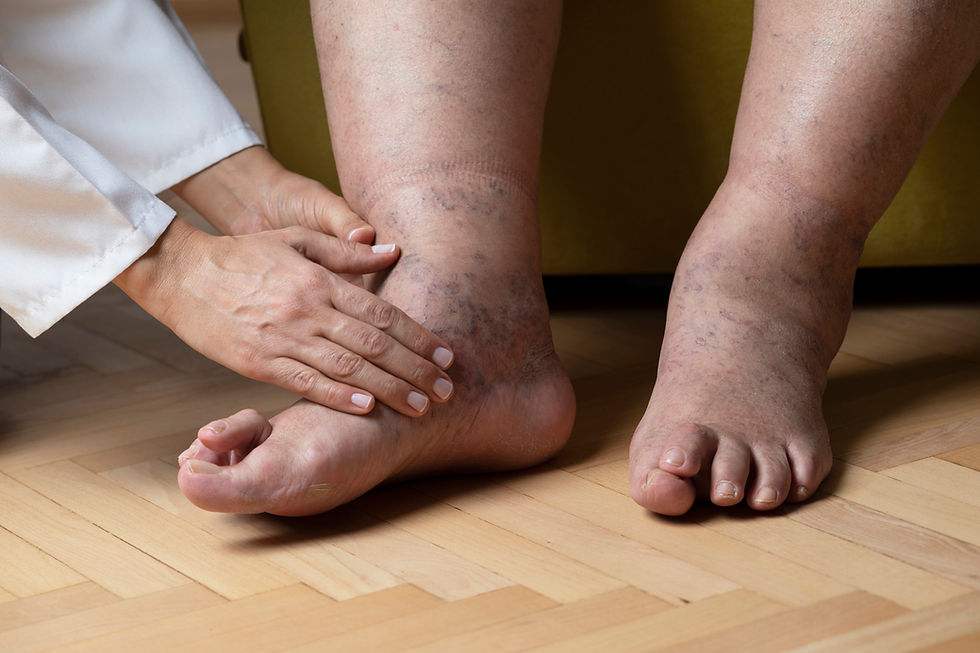
Hundreds of thousands of Americans over the age of 65 who require compression garments to live comfortably with lymphedema will finally have these medically necessary items covered by Medicare starting January 1, 2024 because of the omnibus spending package that passed on Dec 22, 2022. Bill S.1315 is a little-known bill that was tacked onto the omnibus spending package after first being introduced to congress in 2010. The bill had been reintroduced every year since and in multiple years, it was the most co-sponsored bill in congress with broad bi-partisan support. After years of tireless advocacy, the bill has finally passed!
Why did it take a special bill for Medicare to be able to cover lymphedema compression treatment supplies?
Traditional Medicare (Part A and Part B) covers a wide range of health services for seniors. Part A covers inpatient hospital care, skilled nursing facility, hospice, lab tests, surgery, and home health care while Part B covers doctor’s appointments, outpatient hospital services, certain home health services, durable medical equipment, and certain other medical and health services not covered by Medicare Part A.
Until the passage of this bill, Medicare couldn’t cover lymphedema compression treatment supplies because they couldn’t be classified under any existing benefit category in the Medicare law. Because lymphedema compression supplies have a lifespan of about six months, they did not meet the longevity requirement for durable medical equipment. They are also not disposable single use products, so they could not be considered an orthotic or prosthetic by Medicare. This will no longer be an issue once S.1315 goes into effect!
Medicare Will Cover Lymphedema Compression Treatment Items
Despite the fact that CMS has repeatedly acknowledged that compression supplies reduce hospital days for our elderly, it has taken decades for them to be covered by Medicare. Now that they will finally be covered, let’s take a look at the details:
Summary of S.1315 bill:
“This bill provides for Medicare coverage of lymphedema compression treatment items.
Specifically, the bill provides for coverage of standard and custom fitted gradient compression garments that are prescribed by a physician or other specified health care professional to treat lymphedema, and other devices determined to be effective in the prevention or treatment of lymphedema.”
As Medicare agents, we are always happy to pass on good coverage news to our clients. If you have any questions about services or items covered by Medicare, please do not hesitate to contact us for a free consultation. We are here to help!
Our independent insurance agents are dedicated to assisting people on Medicare and those who are ready to transition from employer coverage to personal retirement coverage. We help kupuna understand their benefits options and apply for additional coverage, as needed. We are the only insurance agency in Hawaii contracted with EVERY Medicare Advantage plan, which means we are able to offer unbiased advice; all at no cost to our clients.
At PBC, our clients are our number one priority and we look forward to getting to know you and your needs. Call us today at (808) 738-4500 to see how we may be of assistance.
.png)



Comments